Anti-Inflammatory Diet for IBD (IBD-AID) Quick-Reference
Q: What is the Anti-Inflammatory Diet for IBD?
A: The IBD-AID was derived (and updated) from the Specific Carbohydrate Diet (SCD), and is a nutritional regimen that is based on:
1. Promoting the beneficial, anti-inflammatory intestinal bacteria with:
○ Vegetables & Fruit
○ Soluble Fiber (steel-cut oats, ground flax seed, lentils, beans)
○ Good protein & fats (beans, nuts, olive oil, avocado, ground flaxseed, fish, soy)
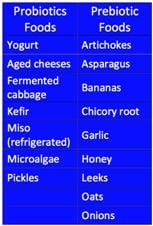
○ Probiotics (yogurt, kefir, miso, kimchi, sauerkraut, local honey)
○ Prebiotics (artichokes, leeks, asparagus)
2. And decreasing the pro-inflammatory intestinal bacteria by eliminating certain carbohydrates, such as:
○ Refined sugars and certain starches
○ Grains (steel-cut and rolled oats are allowed)
○ Lactose (anything containing milk or cream)
These carbohydrates are thought to provide a food for pro-inflammatory bacteria.
3. Together, the foods in this diet decrease bowel inflammation, aid in the repair of the gut, and help to restore balance to the immune system.
Q: How is IBD-AID different from the Specific Carbohydrate Diet or the Paleo Diet?
A: There are many similarities, but IBD-AID emphasizes probiotics, foods with live bacteria within them such as yogurt and miso (see table), as well as prebiotic foods (which feed your good bacteria). This change was made because research shows that IBD patients have more bad bacteria in their gut which contribute to inflammation. This diet helps to restore balance between helpful and harmful bacteria. The diet also differs in that it gradually introduces patients to more textured foods according to phases.
 In addition, IBD-AID emphasizes the importance of fiber, specifically soluble fiber, which helps increase beneficial short chain fatty acids as well as providing a gel matrix to enhance stool consistency and slow gut motility. This means decreased inflammation, more formed and regular bowel movements. Because we recognize the importance of soluble fiber, we allow steel-cut and rolled oats on the diet (SCD does not allow grains of any kind).
In addition, IBD-AID emphasizes the importance of fiber, specifically soluble fiber, which helps increase beneficial short chain fatty acids as well as providing a gel matrix to enhance stool consistency and slow gut motility. This means decreased inflammation, more formed and regular bowel movements. Because we recognize the importance of soluble fiber, we allow steel-cut and rolled oats on the diet (SCD does not allow grains of any kind).
Finally, IBD-AID also recommends certain types of proteins— lean meats, beans, and soy products (tofu)—which are lower in saturated fat. In our experience, patients have tolerated soy well (SCD advises against soy).
In comparison, the Paleo Diet eliminates legumes (all beans, lentils, peanuts), all grains, and all dairy. Otherwise food suggestions and exclusions are similar to those in IBD-AID.
Q: What foods should I avoid?
A: Choose the foods in the pyramid below instead of items with the following ingredients:
- Trans fats (store-bought baked goods, anything containing “partially hydrogenated oil”)
- All foods with refined sugar
- Grains, except for oats
- Fast food or processed food
- Milk & fresh cheeses (aged cheese is ok)
Q: Can I drink alcohol, coffee, and/or tea on this diet?
A: If you do not drink alcohol, there is no reason to change. If you do, we recommend limiting your intake to 1 drink a day for women and up to 2 for men, preferably wine. Beer is not allowed due to its grain content. Coffee and tea are allowed in moderation, but please use non-dairy milk and allowed sweeteners, such as honey or maple syrup.
Q: How can I make IBD-AID an efficient, routine part of my lifestyle?
A: We provide sample meal recipes and ideas, however we will work with you to make this diet a doable part of your often busy lifestyle by modifying recipes and streamlining preparation. Some ideas for quick breakfasts and lunches are below:
- For breakfast, make an easy egg scramble. Sauté vegetables (such as onions, broccoli, spinach, etc.) in a small amount of coconut or olive oil; then add 1-2 eggs, scramble and enjoy!
- For people who need to pack lunches and don’t have time to prepare recipes, salad lunches are perfect. At the beginning of the week, make a huge salad with produce that won’t spoil by the end of the week (such as spinach, mixed greens, bell peppers, cucumbers, carrots, walnuts, almonds, etc), and store in large airtight container. Each morning add on toppings, such as avocados, sliced fresh fruit, grilled chicken, fish, etc. Toss with a homemade salad dressing, or simply olive oil, vinegar or lemon juice, and you are good to go! In addition, we can teach you to make an IBD-AID-friendly sandwich bread.
- Saving leftovers can be helpful for planning meals for the next day, if refrigerated properly. Many slow-cooked (“crock pot”) meals are very useful in this regard.
- Buying fresh is good, but frozen produce is economical, long-lasting, quicker to prepare, and tastes great!
Phases of the IBD-AID diet and how they relate to your symptoms
-How do I know which phase of the diet is right for me?
Please check with a research team member to see which phase of the diet you should be starting in or if you have any other questions.
-
Please check with a dietitian to see which phase of the diet you should be starting in or if you have any other questions.
Phase 1: Bringing it back to basics
If you are currently experiencing a flare or any bleeding, you should select foods from the Phase 1 portion of the diet. This phase of the diet is appropriate for those experiencing urgency and frequency of bowel movements or pain, and is helpful for patients who have recently been hospitalized. At this stage, you may not be able to tolerate many foods. In particular, the texture of the food is important. This phase emphasizes soft-cooked or pureed food using a blender, depending on your personal tolerance.
Example foods: smoothies, well-cooked steel cut oatmeal, ground flax or chia seeds (if you can tolerate ground seeds – see below) pureed soups, pureed vegetables, yogurt and miso (good sources of probiotics), and ground lean meats
Phase 2: Introduction of more foods and textures
Your symptoms have improved significantly, but you may still be experiencing some symptoms. At this stage you may be able to tolerate some fiber, but may still have some difficulty digesting foods very high in fiber or fat. More fibrous foods are added in this phase, in the form of soft cooked vegetables and pureed beans/lentils. Use the foods list as a guide to help you advance to this stage. Remember to drink plenty of water and increase probiotic foods when adding fiber to your diet!
Examples of foods to add at this phase: soft greens (butter lettuce, cooked collard greens, baby spinach without stems), well-cooked lean meats, aged cheeses, nut butters, tomatoes, pureed berries with seeds strained out, and foods baked with IBD-AID friendly flours (bean flour, nut flours).
Phase 3: Remission
You are feeling stronger and are becoming more comfortable eating a greater variety of foods. Your bowel movements are well controlled and solid.
Examples of foods to add: stir-fried vegetables and meats, shellfish, citrus fruits, whole beans, and apples (ideally cooked).
Note: Each person’s ability to tolerate foods will be different, and foods will have to be added or removed from the diet depending on your individual tolerance. Please discuss any dietary questions with your dietitian. When adding new foods, it is normal to experience some mild stomach upset. However, if you notice a continued increase in bowel frequency/urgency or a prolonged decrease in the quality of your stools, please consider removing the new food from your diet or talking with your dietitian.
For recipe ideas, see our IBD-AID Recipe website: http://www.umassmed.edu/Content.aspx?id=148562
Notes: Each person’s ability to tolerate foods will be different, and foods will have to be added or removed from the diet depending on your individual tolerance. Please discuss any dietary questions with the research nutritionists. When adding new foods, it is normal to experience some mild stomach upset. However, if you notice a continued increase in bowel frequency/urgency or a prolonged decrease in the quality of your stools, please consider removing the new food from your diet or talking with the research nutritionists
Examples of IBD-AID friendly recipes
**All phases build upon each other and foods specified for earlier phases can also be eaten in later phases: Phase I recipes can be used in Phase II and III. Phase II recipes can be used in Phase III etc.
Phase I (Also appropriate for Phase II& III)
Breakfast
Banana Oatie Smoothie
Greek Yogurt or Kefir (Optional: with maple syrup or honey)
Lunch
Caribbean Avocado Soup
Carrot and Coriander Soup
Nonnie’s Zucchini Omelette
Dinner
Baked Fish in a Parcel with Miso Sauce
Iron-rich Shepherd’s Pie with Sweet Potato Topping
Leftover Roast Chicken Soup
Snacks and dessert
Quick & Easy Pumpkin Treat
Homemade Chocolates
Phase II (Also appropriate for Phase III)
Breakfast
Slow-Cooker Steel-Cut Oatmeal
Banana Almond Oat Pancakes
Avocado, Spinach, and Cheese Scramble
Scrambled Tofu
Early Morning Smoothie
Lunch
Butternut Squash Bisque
Watermelon and Microgreens Salad
Sue’s Stuffed Mushrooms
Dinner
Roast chicken
Tofu Stir Fry with Zesty Almond Sauce
Spaghetti Squash with Tomatoes, Basil, & Farmer’s Cheese
Snacks and desserts
Mango Salsa
Cheddar Cheese Crackers
Banana Muffins
Maple and Vanilla Roasted Pears
Phase III
Breakfast
Kale & Fruit Smoothie
Frittata with Squash and Celeriac Home Fries
Gluten-Free Granola and Yogurt
Lunch
Red Pepper and Tomato Soup
Mediterranean Chickpeas and Vegetables
Coconut Curry Red Lentil Soup
Dinner
Cannellini Beans with Kale and Walnuts
Chickpeas With Sole And Spinach
Tofu Stir Fry with Miso Sauce
Desserts and Snacks
Cinnamon Apple Muffins
Guacamole and Cheddar Cheese Crackers
How to make IBD-AID an efficient, routine part of your life
- Get prepared
- We have developed menus, shopping lists, and recipes.
- Join an IBD-AID cooking class.
- Keep a food log with symptoms.
- Do not hesitate to email/call your dietitian with questions. We will work with you to make modifications.
- Relax
- This diet provides excellent nutrition and the whole family can be eating the same things you do.
- There will be times you fall off the IBD-AID but it is important to get back on track. We aim for a diet of 80% compliance.
- Ask Questions