General Information
The Family Health Center of Worcester / University of Massachusetts Department of Family Medicine and Community Health Primary Care Psychiatry Fellowship seeks to meet the growing need for improved access to outpatient psychiatric care in the United States, particularly among structurally-marginalized populations, through an intensive one-year training program based in an urban community health center and affiliated academic medical center. 
In 1999, Dr. David Satcher, then the U.S. Surgeon General (left), released a landmark report on Mental Health in the United States in which he repudiated, “the destructive split between ‘mental’ and ‘physical’ health.” This paradigm had created a pervasive stigma surrounding issues of mental health and artificially segregated non-psychiatrists from the mental health of their patients. The surgeon general followed this in 2001 with a subsequent report on Mental Health: Culture, Race, and Ethnicity, in which he argued that this dynamic is frequently exacerbated by deeply entrenched disparities in access to mental health care along lines of race, culture, class, gender, age, housing and insurance status. In pursuit of parity, Dr. Satcher emphasized the essential role of primary care providers in identifying, linking to care, and treating individuals living with mental illnesses.
Nearly twenty years later, advances have been made on the policy level. The Mental Health Parity and Addiction Equity Act mandated reimbursement for mental health treatment on par with that for medical or surgical interventions. The Patient Protection and Affordable Care Act included mental health and substance use treatment as one of ten essential benefits for Medicaid and marketplace plans. It also provided funding for the integration of behavioral health into health centers and primary care clinics.
While policy advances have done much to address those disparities in access to care that Dr. Satcher discussed at the close of the last century, they have been woefully insufficient to the scale of the problem. It is estimated that 40 percent of patients seen in a typical day by their primary care provider have an active psychiatric condition. Studies have also shown that 50 percent of patients referred to psychiatry by their primary care provider (PCP) will be unable to access those services. This is in no small part because 77 percent of counties in the US have a severe shortage of psychiatrists. Unfortunately, the supply issue appears to be worsening even as demand increases. According to the National Council for Behavioral Health, there were ten percent fewer psychiatrists per capita in 2013 than there had been a decade earlier. In this context, it becomes even more important for PCPs to broaden their understanding of what they can and should consider treating within their clinics, particularly for medically underserved populations who face significant barriers in having their mental health needs met.
Health Professional Shortage Areas: Mental Health Providers by County 2022
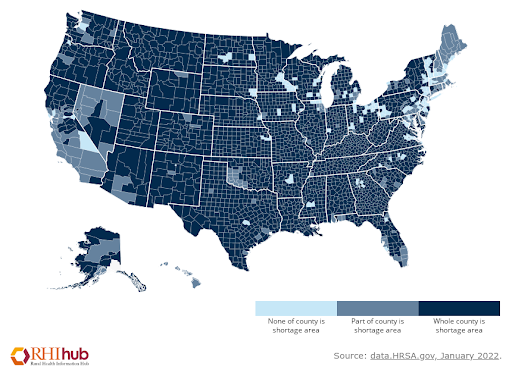 Chart demonstrating counties across the United States designated as full or partial Health Professional Shortage Areas (HPSA) for Mental Health Providers.
Chart demonstrating counties across the United States designated as full or partial Health Professional Shortage Areas (HPSA) for Mental Health Providers.
Family medicine has long been a specialty that is responsive to the needs of its communities and adaptive to acquiring the skills necessary to address those deficits. Unfortunately, while most primary care providers complete their post-graduate training with some experience managing uncomplicated depression and anxiety, overall training in the diagnosis and treatment of psychiatric conditions is often suboptimal to meet patients’ needs. Primary care providers with a more robust knowledge of common psychiatric conditions, including depression, anxiety, substance use disorders, bipolar disorder, attention deficit/hyperactivity disorder, obsessive-compulsive disorders, and some psychotic disorders would provide their practices with an invaluable resource to manage a greater portion of their patients’ psychiatric care needs while also providing more flexibility than consulting specialists can typically offer. Given the impact of untreated psychiatric conditions on physical health as well as the side effect profiles of many psychotropic medications that impact cardiovascular and metabolic health, physicians trained in primary care psychiatry are also in an ideal position to provide comprehensive care to their patients.
While primary care providers cannot and should not supplant the role of psychiatrists, a greater overlap in scope of practice is essential to meeting community need while also allowing psychiatrists to focus on more complex cases. Not only do personality, cognition, and mood impact physical health and functioning, they also interconnect with the individual’s social situation. Integrating primary care and psychiatry through expansion of the training of PCPs has the potential to drastically improve access to mental health care, reduce the stigma of mental illnesses, and foster deeper relationships between provider and patient.  Dora Rivera, LPN, Team 3 Lead Nurse at Family Health Center of Worcester, who provides clinical and logistical support to the fellowship. Photo by An-Hoa Giang, MD, for the Workers of Worcester project.
Dora Rivera, LPN, Team 3 Lead Nurse at Family Health Center of Worcester, who provides clinical and logistical support to the fellowship. Photo by An-Hoa Giang, MD, for the Workers of Worcester project.