Pamela Howes

Pamela Howes, a 56 year old school teacher who suffered a subarachnoid hemorrhage in 2010.
I always felt healthy and energetic, enjoying my life in every aspect. I was teaching my 8th grade English classes, attending graduate school part-time, reading for pleasure, going to yoga, petting my cat and enjoying the time spent with family and friends.
Around Christmas time in 2009, I started having headache that kept getting worse over the course of ten days. I visited my doctor and an MRI of my brain was unremarkable shortly before the morning when I awoke in unbearable pain. I called my parents who lived close by. My father came to my house and called for an ambulance immediately. The last thing I remember is waving to my father from the ambulance window trying to reassure him that things would be alright.
The ambulance took me to a local hospital where shortly after I arrived I became unresponsive and my heart stopped beating; I went into cardiac arrest. I was successfully resuscitated and intubated. A CT scan of my brain showed massive and diffuse subarachnoid hemorrhage.
I was then flown to UMass Hospital, where on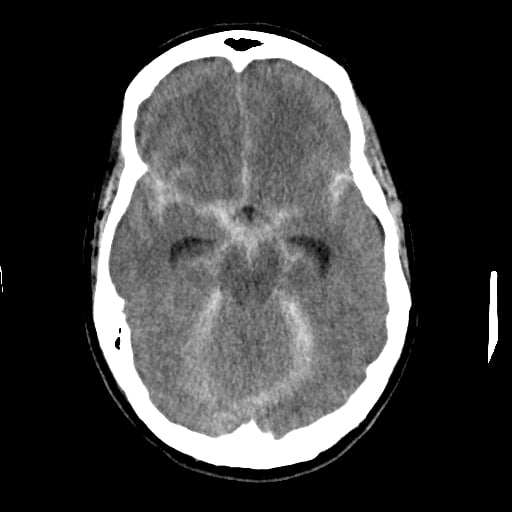 arrival I remained unresponsive and another CT scan of my brain showed that the bleeding was getting worse. It showed an evidence of obstruction of the spinal fluid (CSF) drainage system by the blood causing increased pressure in my head. A neurosurgeon placed an EVD (Extra-Ventricular Device) to drain the blood and the CSF and relieve the pressure, right after that I underwent a cerebral angiogram procedure (similar to a heart cath as a technique but it images and intervenes on the brain arteries instead), they found a 3.2 mm x 3.4 mm aneurysm in the left side of my brain outpouching off an artery called the left posterior communicating artery (PComm.), the aneurysm was successfully coiled. While in the angiography suite, my blood pressure dropped and the oxygen level dropped too. They had to put me on vasopressors to raise my blood pressure. I was having large amounts of frothy secretions coming out of my airways. A central venous catheter was placed in my right internal jugular vein emergently and another catheter was placed in my femoral artery to monitor my blood pressure. An echo of my heart showed a weakened muscle pumping only 15% (normal is ≥ 55%). I was then in the Neurological Intensive Care Unit for three weeks. My blood pressure continued to drop and I was again on more medications to raise my blood pressure. My heart enzymes have already started to increase and the echocardiogram showed a globally reduced contraction consistent with stress-induced cardiomyopathy or what is referred to sometimes as “broken heart syndrome”, but it won’t give up on me nor would the doctors and the staff in the NeuroICU. My blood pressure continued to drop and more IV medications to raise it couldn’t do the job, the other organs in my body weren’t getting enough blood supply or oxygen. They called a cardiac surgeon who placed an intra-aortic balloon pump to take off some of the load on my heart and augment blood supply to my organs. Within 48 hours I was successfully weaned off the intra-aortic balloon pump.
arrival I remained unresponsive and another CT scan of my brain showed that the bleeding was getting worse. It showed an evidence of obstruction of the spinal fluid (CSF) drainage system by the blood causing increased pressure in my head. A neurosurgeon placed an EVD (Extra-Ventricular Device) to drain the blood and the CSF and relieve the pressure, right after that I underwent a cerebral angiogram procedure (similar to a heart cath as a technique but it images and intervenes on the brain arteries instead), they found a 3.2 mm x 3.4 mm aneurysm in the left side of my brain outpouching off an artery called the left posterior communicating artery (PComm.), the aneurysm was successfully coiled. While in the angiography suite, my blood pressure dropped and the oxygen level dropped too. They had to put me on vasopressors to raise my blood pressure. I was having large amounts of frothy secretions coming out of my airways. A central venous catheter was placed in my right internal jugular vein emergently and another catheter was placed in my femoral artery to monitor my blood pressure. An echo of my heart showed a weakened muscle pumping only 15% (normal is ≥ 55%). I was then in the Neurological Intensive Care Unit for three weeks. My blood pressure continued to drop and I was again on more medications to raise my blood pressure. My heart enzymes have already started to increase and the echocardiogram showed a globally reduced contraction consistent with stress-induced cardiomyopathy or what is referred to sometimes as “broken heart syndrome”, but it won’t give up on me nor would the doctors and the staff in the NeuroICU. My blood pressure continued to drop and more IV medications to raise it couldn’t do the job, the other organs in my body weren’t getting enough blood supply or oxygen. They called a cardiac surgeon who placed an intra-aortic balloon pump to take off some of the load on my heart and augment blood supply to my organs. Within 48 hours I was successfully weaned off the intra-aortic balloon pump.
I was already put on medications to prevent seizure and on antibiotics to treat pneumonia. The pressure in my head was rising threatening my brain to herniate, but I was treated successfully for that. My legs stopped moving, and a Doppler ultrasound of the brain vessels showed diffuse constriction of the arteries referred to as vasospasm, yet another complication of the subarachnoid hemorrhage, and I again underwent cerebral angiogram where a medication infused in the brain arteries to successfully relieve that vasospasm. A CT scan and MRI of the brain showed multiple areas of stroke in my brain, but none affecting my language center or motor control areas. After that it was a matter of time to start improving with the extraordinary care from the team of doctors, nurses and other staff in the Neuro ICU. I left after three weeks of a miraculous journey to continue recovering in a rehabilitation center.
In September of 2010, I was weaned off all  but one or two medications. I was back to my school teaching part time. In September, 2011, I was back teaching full time. By the fall of 2012, I was back in graduate school and finished my degree in two years. I have returned to yoga, continue my love of reading, and petting my, now, two cats. I do these things all in the beauty of life in the heart of New England.
but one or two medications. I was back to my school teaching part time. In September, 2011, I was back teaching full time. By the fall of 2012, I was back in graduate school and finished my degree in two years. I have returned to yoga, continue my love of reading, and petting my, now, two cats. I do these things all in the beauty of life in the heart of New England.
As my journey of recovery continues, I have been most affected in two ways. First, I have been impressed with the lack of awareness of brain injuries. It is very much an invisible disability. While sympathy is aplenty, knowledge about it is scarce in the community. I work to educate those around me as I best can. But, more significantly on this journey, I have found myself living my life with more gratitude than ever before. The list of people and things for which I am grateful is very long, I am especially thankful to the team of doctors, nurses and other staff at UMass Neuro ICU for the wonderful care they provide.
May this story I share give hope to those in need. Coming back from a brain injury is possible. I especially thank the doctors and other care providers who dedicate their lives to make such a possibility exist.
