Standardized Patient Program
Standardized Patient Program
UMass Chan Medical School iCELS Standardized Patient (SP) Program began in 1982 under the leadership of renowned medical education pioneer Dr. Paula L. Stillman, M.D.. Today, UMass Chan has one of the longest running SP programs in the United States, serving multiple programs in the New England region and beyond.
Standardized patients are everyday people who are trained to consistently simulate medical conditions in a medically accurate and emotionally authentic way, to support your learners' education goals. More than 100 standardized patients in the program represents a microcosm of today's patient population. Our SPs undergo rigorous foundational training to acquire core SP competencies, before undergoing further training on specific case scenarios. This ensures effective portrayal, assessment, and sharing of feedback by the SPs, to support effective learning among medical students, nursing students, nurse practitioner candidates, physician assistant candidates, therapists, residents, researchers, practicing clinicians and more.
Please select a topic for shortcut to its respective section:











Types of SP Sessions
 Over the years, depending on the scope of duty at each assignment, Standardized Patients (SPs) have also been referred to by various healthcare professionals as:
Over the years, depending on the scope of duty at each assignment, Standardized Patients (SPs) have also been referred to by various healthcare professionals as:
- Standardized Participants (SPs)
- Standardized Persons (SPs)
- Simulated Patients (SPs)
- Professional Patients
- Patient Actors
- Patient Models
- Patient Instructors
- Physical Exam (PE) Instructors
- Physical Exam Teaching Associates (PETAs)
- Gynecological Teaching Associates (GTAs)
- Genitounitary Teaching Associates (GUTAs)
- Male Genitounitary Teaching Associates (MUTAs)
What all these SPs have in common are that they receive professional core competency skill as well as specific case scenario trainings before teaming up with clinical faculty to assist learners with their mastery of clinical skills in high and low stakes examinations, small group teaching sessions, and one-on-one specialized clinical electives. Examples of SP participations include:
- SP in one-on-one encounter with a learner who is practising comprehensive historytaking, focused physical exam, clinical reasoning and patient consultation
- SP in one-on-one encounter with a group of learners who are practising communication skills around delicate subjects such as end-of-life care, intimate partner violence, and substance use disorder including opioids dependency
- SPs in a family conference with an inter-professional healthcare team
- SPs in a hybrid scenario involving high-fidelity human patient manikins, where the learner(s) learn to deal with multiple challenging elements during an emergency situation
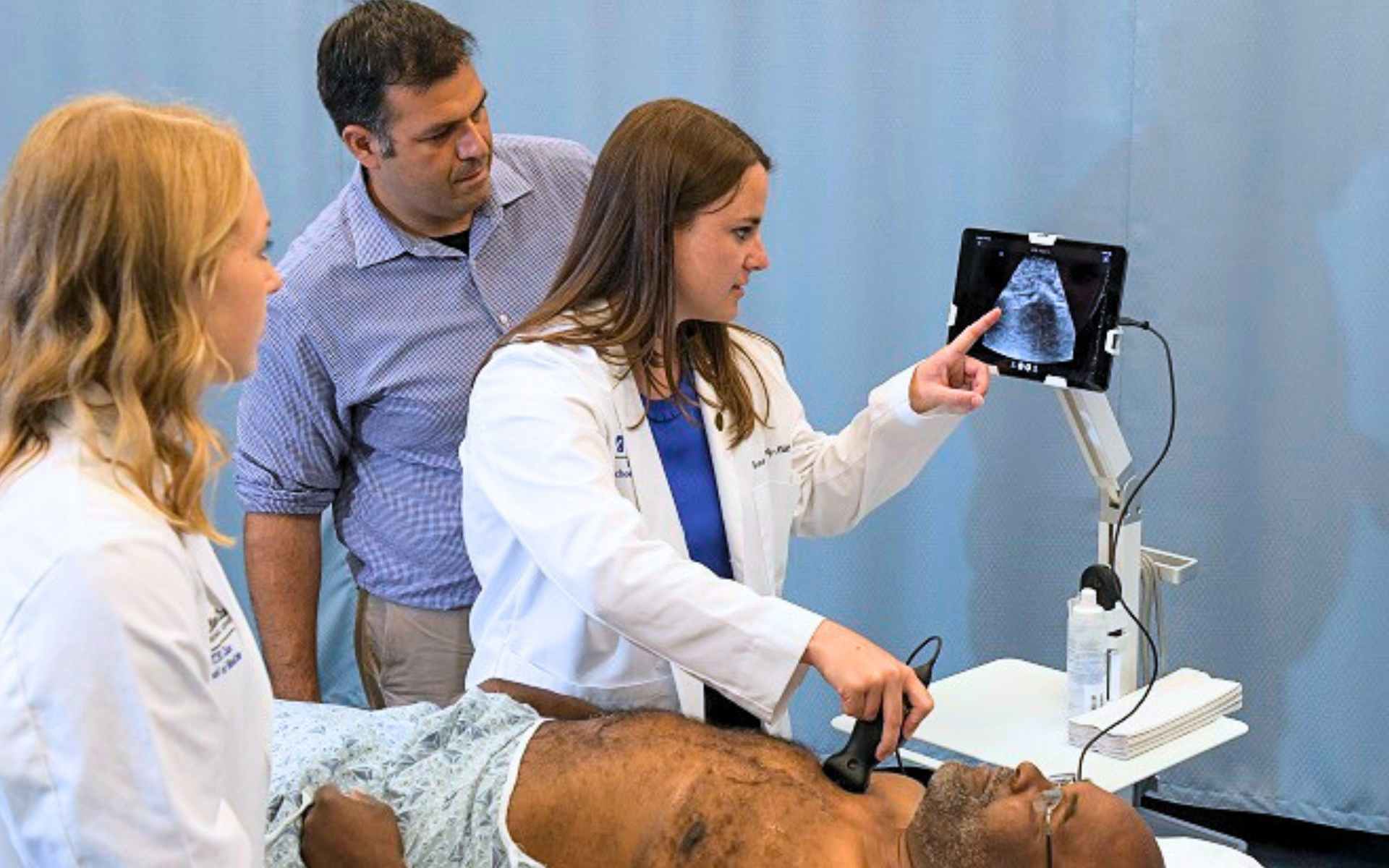
- SP as a healthy patient model at ultrasound sessions including Point of Care Ultrasound (POCUS) which are currently receiving a lot of attention
- SP as a physical exam instructor who has been certified to observe, assess, and demonstrate correct ways to carry out specific physical exams - including focused exams, full body exams covering approximately 200 maneuvers, and specialized genitourinary exams on both healthy male and female patients
UMass Chan Medical School iCELS works closely with faculty to pre-determine the complexity, scope, and duration of each encounter with the SPs.
SPs in Clinical Encounters
In this commonly-recognized format, the SPs are trained to portray real patients who are experiencing a specific clinical scenario as pre-defined by the faculty, to meet the learner's learning objectives. An SP may be in gown, with moulage (medical make-up to mimic specific conditions), displaying specific affects, and seated in a wheelchair. However, an SP's role goes beyond portrayal - SPs master the case scenario including the patient's History of Present Illness (HPI), Past Medical History, Social History, Family History, and accurate responses to give during Focused Physical Exams, to immerse the learners in a realistic encounter. During this encounter, SPs are also actively observing and assessing the learner's approaches and responses, for scoring and feedback after the encounter. Deliberate practice of areas identified for improvement may take place during feedback session, to further enhance learning outcomes. At all times, SPs adhere to professional standards on medical accuracy, emotional authenticity, and the providence of an inclusive as well as supportive learning environment.
Studies have found SPs to be effective in teaching clinical, interviewing and communication skills to learners from a variety of disciplines, including medicine, nursing, dental, law and other professions. Authentic, first-person-perspective feedback from the SPs have also been shown to be particuarly effective in helping medical students acquire empathy and communication skills.
At UMass Chan Medical School iCELS, SPs have also been trained on assessing the quality of communication using the Master Interview Rating Scale, an industry standard that determines if a healthcare provider has used effective types of questions, pacing, facilitative skills, positive reinforcements, transitions, opportunites for the patient to ask questions, closing, and more.
SPs in Hybrid Scenarios
SPs can also be paired with manikins, whereby the SPs would provide feedback on communication and interpersonal skills, while the manikins' presence provides the learners with opportunities to practice technical skills that are too invasive to perform on a real human. Examples of Hybrid Scenarios include:
- An SP as the patient, and a pelvic model task trainer for the learner to perform gynecological exam on during the clinical encounter
- An SP as the patient's relative, and a full sized human patient manikin as the patient who is demonstrating complex symptomes and vital signs
When meticulously designed and closely coordinated, Hybrid Scenarios can bring ultra-realism to the case scenario, thus providing a level of learning that exceeds that provided by each modality alone. The list of manikins, task trainers, and other clinical inventories that can be paired with an SP is extensive. Find out more about Hybrid Scenarios in our Simulation Lab section.
SPs As Physical Exam (PE) Instructors
A Physical Exam (PE) Instructor, also known as a Physical Examination Teaching Associate (PETA), is a highly-trained Standardized Patient who has completed our internal certification process, to observe, assess, and teach healthcare learners how to perform full body physical examinations on patients.
Areas include: Head, ears, eyes, nose, oral, and throat (HEENoT), breast, heart and lungs, the abdominals, musculoskeletal and neurological exams - commonly, a full body physical exam session may cover approximately 200 maveuvers including the correct use of instruments such as the othalmoscope, otoscope, blood pressure cuffs, which the PE Instructor can assist the learner with where necessary.
PE Instructors use their professional knowledge of anatomy, physiology, and clinical skills, as well as their first hand perspective as a patient themselves, to provide clear feedback and supportive guidance on the accuracy, completeness, safety, comfort, dignity, and communication aspects of the exam. Valuable opportunities for deliberate practice would also be identified to suit the needs and preferences of individual learners, further entrenching the learning outcome in this supportive and controlled learning environment.
Some of the most heartfelt feedbacks that iCELS has received from our learners, have been a direct result of these highly-valuable, hands-on, individual training sessions!
SPs As Genitourinary Instructors
Gynecological / Genitourinary / Male
Genitourinary Teaching Associates (GTA, GUTA, MUTA)
A Gynecological Teaching Associate (GTA), Genitourinary Teaching Associate (GUTA), or Male Genitourinary Teaching Associates (MUTA), is a person who is trained to teach medical students and other health professionals how to perform sensitive examinations of the genital and urinary systems.
iCELS is proud to be home to a support system that provides a confidential and conducive learning environment for a highly-specialized team of GTAs/GUTAs/MUTAs to professionally foster the learners' development of essential communication skills, professionalism, and ethics when accurately carrying out sensitive genitourinary examinations.
GTAs/GUTAs/MUTAs are trained to a high level of comfort and confidence in faciliating an essential education session with their own body, while maintaining confidentiality and boundaries with learners, as well as respect and empathy for the diversity of others. A strong sense of professionalism is emphased on how to provide constructive feedback and guidance to learners in a respectful and supportive manner.
Speak to us to discover the high-value learning that takes place at these GTA/GUTA/MUTA sessions since our program's founding in 1982!
SPs As Patient Models For Ultrasound Sessions
iCELS has a large pool of SPs who have been introduced to the use of ultrasound, including the portable or handheld Point-of-Care Ultrasound (POCUS) devices, as a noninvasive diagnostic procedure that healthcare providers can practice on them for. Our SPs are familiar with proper attire in hospital gowns and ready to cooperate by providing adequate access for the ultrasound session.
Areas include: Neck, chest, upper extremity, back, abdomen, bladder, leg, and knee. iCELS SPs have also been briefed on the level of access required for Extended Focused Assessment Sonography in Trauma (eFast), Focus Assessed Transthoracic Echocardiography (FATE), Deep Vein Thrombosis (DVT), and Lumbar Puncture ultrasound (to find physical landmark only, without actual lumbar puncture). At this time, these ultrasound sessions do not include the genitourinary organs.
The ultrasound session is more than a practice: While SPs may be accustomed to the idea of feeling cold from the ultrasound gel, they have also been encouraged to communicate professionally and effectively if they feel pain from the pressure being applied. This simulates realistic clinical scenarios, and the SPs' sharing of insights with the learners provide constructive feedback to enrich the learning ahead of real-world applications today.
Customize Your Simulation
UMass Chan Medical School’s interprofessional Center for Experiential Learning and Simulation (iCELS) collaborates with departments and faculty, both from UMass Chan and external organizations, to deliver an exceptional depth of resources and professional services grounded in the use of our facilities and services, to serve the needs of medical, nursing, and allied health clinician, educator, as well as researcher communities.
Holding extensive experience in providing assessment, consultation, and support in running simulation sessions in and beyond our immediate geographical location, our team is ready to collaborate on new projects with you to customize or develop curriculum, build scenarios, create skills workshops, and teach you how to use the equipment as well as carry out effective debriefing to meet learning goals and objectives.
Talk to us today about the right mix of sim modalities to meet the needs of your learners. Your can get started by visiting this section on Consulting to Customize & Create Your Own Healthcare Simulation Session.
Locations of SP Sessions
These sessions can be held at your venue, ours, or online. The iCELS team is experienced in despatching our team of highly-trained SPs to client venues in Boston, Worcester, Springfield, and beyond.
At our venue, iCELS occupies a 24,000 sq ft space at the UMass Chan Medical School Campus Albert Sherman Center (ASC). 20 patient exam rooms, complete with adjustable exam beds and fitted with working otoscopes, ophthalmoscopes, blood pressure monitors as well as sanitizers and essential clinical supplies, are ready to immerse your learners in an authentic learning experience that closely mimics real world settings. All 20 patient exam rooms are equipped with cameras and microphones for live viewing as well as video recording on CAE LearningSpace for post-encounter reviews.
If an online encounter is most suitable for your case scenario, UMass Chan Medical School iCELS is also pleased to have also amassed high volume experience in carrying out a broad range of Standardized Patient encounters online.
How SP Programs Work For You
STEP 1: Gather Information
Let us know about the learning objectives, type and number of learners, target dates, and all relevant aspects of your education session.
STEP 2: Write Case Scenarios
Almost all SP sessions involve case scenarios. In this respect, we will support you with case templates and case samples, as well as schedule and setup recommendations for your session to achieve optimal outcomes. In the alternative scenario where you are hiring the SPs for a Physical Examination Training session or a Point of Care Ultrasound (POCUS) session which do not involve case scenarios, this step might not apply.
STEP 3: Case Training, Finalizing Details
SPs who have completed their foundational skills training (or are specifically recruited from the local community for your project) would be scheduled for the assignment, and further trained for 2 hours to master the case scenarios where provided. This further training also serves as a rehearsal for the actual encounter, and can be very effective in spotting any information gaps that need to be finalized or details that need to be standardized, to deliver a medically accurate and emotionally authentic education session to your learners.
STEP 4: Confirming Learners' Attendance
At this point, your learners' schedules should be finalized and all logistical details conveyed for smooth-running on the actual day of the simulation event.
STEP 5: Simulation and Debrief with the Learners
Education event takes place - whether online or onsite, at your venue or ours, with or without recording, scoring and post-encounter feedback from the SPs. We recommend and support the use of debriefing as an essential component of learning through simulation. It involves learner self-reflection as well as postive and constructive feedback from the SPs about the learners' performance, to faciliate positive and desirable development in the learners.
How Do SPs Support Faculty-Determined Education Goals?
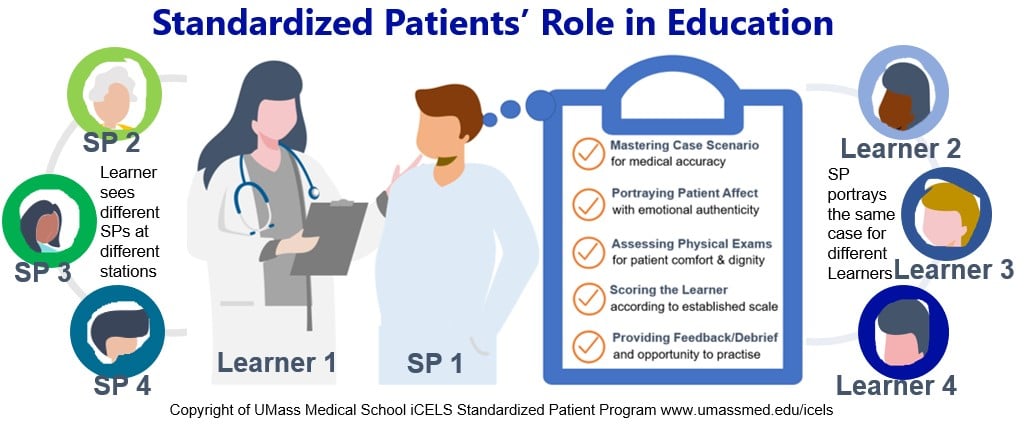
Example of an education event involving a circuit of 4 scenarios: Learner 1 sees SP 1, followed by SP 2, SP 3 and SP 4 at this circuit. Each SP presents a different case scenario for the learner to practice, get assessed, and receive feedback on. Meanwhile, SP 1 sees Learner 1, followed by Learner 2, Learner 3 and Learner 4.
Our Standardized Patients can help meet your education goals by:
-
-
Mastering case scenario as provided by your faculty. All SPs who are portraying the same case are trained together and our performance calibrated, with the support of our proprietary reference system which includes the use of a Case Cornerstone and Memory Tools. This helps SPs deliver detailed scenarios with medical accuracy.
-
Portraying patient affect - including replicating the manifestations of conditions, emotions and communication challenges - with emotional authenticity to engage the learners in realism. At an Objective Structured Clinical Examination (OSCE) circuit, the SP would do this for one learner after another, with breaks in between.
-
Assessing focused physical examinations (PEs) carried out by the learner for accuracy of maneuver, patient comfort and dignity during the encounter.
We also have a specialized team of SPs who are certified Physical Examination Teaching Associates (PETA) a.k.a. PE Instructors to help learners master full body physical exams involving ~200+ checkpoints, as well as highly experienced Gynecological / Genitourinary / Male Teaching Associates (GTA, GUTA, MUTA) to help learners master the finepoints in conducting breast, pelvic, genitourinary and digital rectal exams with great care, accuracy and sensitivity towards the patients' needs, ahead of their encounter with actual patients. -
Scoring and documenting learners' performance according to established scales which may include, but are not limited to, the Master Interview Rating Scale (MIRS). MIRS is a published and validated instrument that rates >20 key aspects of a learner's communication skills using a Likert Scale. Learners may be rated for their non-verbal facilitative behavior, verbalized empathy, pacing, transitions from one subject to another, use of jargons, questioning techniques, and more. The SPs are also familiar with documenting the learners' performance on your preferred platform, online or physical forms, or CAE LearningSpace where available.
- Providing feedback or debrief in accordance with established methods. This include the use of self reflections, as well as individualized feedback starting with positives observations, adding suggestions for improvement, and closing with a summary that includes positive encouragements. SPs are also trained to quote specific examples of behaviors so learners can take part in a deliberate practice. Our aim is to provide a learner-centric experience to support your education goals.
-
How Are UMass Chan SPs Prepared For Their Roles?

In order to maintain a high standard of educational excellence, SPs at iCELS undergo a series of foundational training as well as event/case-specific training before they see your learners at an encounter. Over time, an SP would attend a series of core competency development training sessions to refine their skills. Experienced SPs would further undergo instructor certification programs so that they can advance on specialized skills to support faculties on the more complex educational needs.
At all times, SPs could be observed and their performance documented as part of an ongoing Quality Assurance (QA) process at iCELS. Video recording of simulations at iCELS facility allows our faculty, staff, trainers and SPs to review past work and assess various aspects of the encounters for improvement.
Once a year, SPs would participate in the Performance Appraisal, during which each of the ~100 SP receives protected time to review their core competencies and continuous development with the iCELS leadership team. This is yet another component of the iCELS focus on continuous quality improvement towards excellence.
We encourage your faculty and learners to provide feedback on what went well and any areas for improvement that our SPs should know about too!
Our Pioneering Experience
The UMass Chan Medical School iCELS Standardized Patient Program was established in 1982 as one of the earliest SP programs around. The program continues to cross many milestones in its size, strength, influence and experience.
Today, the utilization of standardized patients as an evaluative and instructional tool has become an integral and mandatory component in all four years of the medical school curriculum – not only at UMass Chan Medical School but at medical schools across Massachusetts. Many SPs who had started with the program in its earlier years remain a source of experience and perspectives to our ongoing approach towards excellence.
Find out about a remarkable pioneering history that took place right here at the UMass Chan Medical School SP program.
Successful Learning Outcomes
We greatly value feedback from clients - and there have many wonderful ones! In respect of confidentiality, clients' names and organizations are omitted:
"As always, the SPs were well-prepared and each of them presented a compelling, highly believable story that helped prepare our students gain comfort and competence in screening their future patients for domestic violence and elder abuse. Once again, the organization, timing and implementation of this exercise, run in 15 rooms, three separate times, and for over 200 learners were absolutely flawless. We are all so fortunate to be the beneficiaries of this excellent educational resource!" - From a Worcester medical school faculty lead
"The faculty’s feedback on all five professional SPs portraying an adolescent was that they were “excellent” and "wonderful". Another home run for the SP program!" - From a Worcester medical school faculty lead
"An abstract I submitted following the previous three years of data collection associated with our OSCEs was accepted. I will be presenting the related poster at the next Association of Standardized Patient Educators (ASPE) conference. Thank you to you and your entire staff for their contributions." - From a Lowell, MA physical therapy program
"Our students had a wonderful experience this year. Thank you!" - From a Boston physician assistant program
"All the actors were wonderful, timely, and just lovely to work with!" - From a Boston medical school's interprofessionalism course faculty
"The students found the experience incredibly beneficial and we have received much positive feedback" - From a Boston social work program
"The actors you arranged for the recording were FANTASTIC." - From a Boston Continuing Medical Education provider, about an educational video about opioids misuse
"The students appreciated the great learning experience. Thanks again for coordinating this opportunity." - From a Springfield, MA midwifery gynecology teaching associate session
"Thanks for a well-organized day. All of you are so welcoming! The OSCEs are very valuable for our students and for our review of our curriculum!" - From a New Hampshire nurse practitioner program's assessment session held at iCELS venue
"The SP and the speakers were great together. We're excited for the rest of the series." - From a Continuing Medical Education provider, regarding an SP simulation session held as part of a symposium in Atlanta, GA; Baltimore, MD; Dearborn, MI; Los Angeles, CA; Minneapolis, MIN; New York, NY; and Rosemont, IL
Meet Our Standardized Patients
A community of ~100 trained and experienced SPs are available for simulation sessions held onsite and online, for UMass Chan as well as many other organizations like yours, to provide an immersive experience to all stages of learners.
Recognizing the importance of serving today's population, and driven by a heart for public health, iCELS is a strong supporter of a diverse and inclusive learning experience. In this respect, we constantly strive to have all genders, ages and races represented in our SP community.
You may find it a welcoming fact too, that many of our SPs are actively engaged in our internal Town Hall Meetings and Working Groups for Quality Improvement, as well as a feedback-anytime process that is designed to gather the voices and values that are truly present in the population around us today. Our aim is to build an SP community that is engaged, informed, and ready to support your education session.
"Meet the SP" articles coming soon.
Frequently Asked Questions
Last updated: Jul 19th, 2023
About iCELS Standardized Patient Program
How do I reserve an SP session?
If this is your first time working with UMass Chan Medical School iCELS SP Progrm, you might be delighted to find out about our established approach and methods at the SP Program section. If you are already familiar with how our program works, the next step is to make a booking at Contact Us section. Our dedicated and experienced team will work closely with you to plan for a successful education session.
How does one become a Standardized Patient?
SPs come from all walks of life, all races, ethnicities, abilities, ages and genders. These are everyday people who form part of an educational team at UMass Chan Medical School, by looking and acting like an actual patient after receive rigorous training provided by us, to accurately and consistently portray the personal history, physical findings as well as personality traits of an individual patient in a realistic and repeatable (standardized) way. SPs receive constant training to help medical learners learn how to interact with patients, and to deliver effective feedback to support a learning session. While some SPs enrich our shared experience with their background in acting, healthcare, education or communication, the SP community really is made up of a diverse range of individuals who are eager to learn and help faculty members carry out simulations to support education goals. Find out more about how one becomes at SP at our popular SP Recruitment section.
I'm very impressed by your SP's performance! How do I submit a compliment?
Thank you for engaging us in your experiential learning session. It gives iCELS and our SP community a great sense of satisfaction to know that we have engaged you in a realistic simulation session to help improve patient experience. Your feedback would help us deliver our best in this eve-advancing field of healthcare in the population today. You are most welcomed to share about the experience by Submitting a Feedback at the Contact Us section!
You might also be interested in: