Fecal Microbiota Transplant (Stool Transplant) to treat Clostridium difficile infections
PI: Randy Pellish, M.D.
Clostridium difficile is commonly found in the environment and in about 5% of all healthy adults. It normally lives harmlessly in small numbers in the gut, and is held in check by a healthy microbiome. If this balance is thrown off, for example following antibiotic treatment that damages the healthy microbiome, the population of Clostridium difficile can expand out of control. In large numbers these bacteria begin to produce toxins, leading to pseudomembranous colitis, diarrhea, toxic megacolon, and possibly sepsis and death.
The prevalence of Clostridium difficile infection (CDI) in patients in US hospitals has increased significantly in recent years, with diagnosis rates of CDI more than doubling from less than 150,000 as of 2001 to more than 300,000 in 2005. In addition to this increase in new cases, there has been an increased incidence of recurrent CDI, in which patients undergo treatment but are unable to fully eradicate the infection and thus have continuing disease episodes. Recurrent CDI cases are more likely to result in hospitalization, and the rate of recurrent CDI is now about 30% for the first recurrence and even higher for subsequent recurrences. As antibiotic treatment during hospitalization for other reasons is a major trigger for CDI, this complication has imposed a major financial burden on the health care system. The cost of treating CDI is rising and was estimated to account for $4.8 billion in excess healthcare costs in acute-care facilities in 2008.
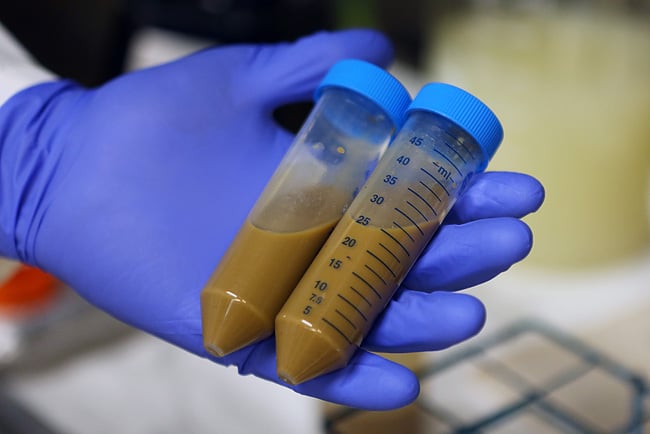 A promising solution to the problem of recurrent CDI is the Fecal Microbiota Transplant (FMT), in which stool is transplanted from a healthy donor into the colon of a CDI patient. There have been multiple case reports describing FMT administered through colonoscopy, retention enema, or nasojejunal tube to treat patients with recurrent CDI who were unresponsive to standard antibiotic therapy. The results thus far have been very promising, with studies showing resolution of patients’ symptoms in about 90% of cases and largely eliminating recurrence. However, most of these studies were small and not carefully controlled and so FMT has not yet become common and acceptable medical practice.
A promising solution to the problem of recurrent CDI is the Fecal Microbiota Transplant (FMT), in which stool is transplanted from a healthy donor into the colon of a CDI patient. There have been multiple case reports describing FMT administered through colonoscopy, retention enema, or nasojejunal tube to treat patients with recurrent CDI who were unresponsive to standard antibiotic therapy. The results thus far have been very promising, with studies showing resolution of patients’ symptoms in about 90% of cases and largely eliminating recurrence. However, most of these studies were small and not carefully controlled and so FMT has not yet become common and acceptable medical practice.
Careful research on FMT is required to assess and improve the success rates, the quality of outcome, and the benefit to patients with CDI. Our current study at UMassMemorial Medical Center is evaluating FMT administered by colonoscopy. We are recruiting patients with recurrent Clostridium difficile infection, who have failed at least one course of antibiotics. The person donating the stool is selected by the patient, and is usually a family member or friend. The stool donor undergoes tests to screen for any possible infectious diseases that could be passed through the stool. The stool is then transplanted to the patients and they are monitored to evaluate the effectiveness of FMT at treating and eliminating the infection. This and other studies will help to evaluate the suitability of FMT as a widespread therapy.