Learn about microbiome research in the CMR
The collection of microbes - and their genes – that inhabit our human body is termed the microbiome. Our gastrointestinal tract alone is home to trillions of bacteria, a population that outnumbers human cells 10 to 1 and has 350 times the genomic material. The microbiome has a profound influence on human health in areas such as immune development, nutrition, and disease.
Research under the CMR umbrella encompasses a wide variety of clinical, translational, and basic science topics. To find out more about the kind of research topics we are tackling, look left and explore our projects under the topics of diet, infectious disease, inflammation and immunity, probiotics, and biofuels. For more information about the microbiome in general, check out the "FACTS" tab above, and to hear from researchers themselves or ask us a question, just go to "TALK".
| TOPICS | |
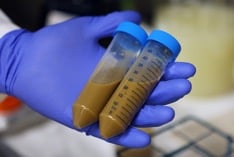 |
Fecal Microbiota Transplant (Stool Transplant) to treat Clostridium difficile infectionsClostridium difficile infections are a major health problem across the United States. Infection occurs when antibiotics disrupt the normal microbiome in the colon, allowing Clostridium difficile bacteria to take over. Killing these bacteria requires even stronger antibiotics, and unfortunately these antibiotics are becoming less effective every year. At UMassMemorial Medical School, we are evaluating the effectiveness of a promising new approach, Fecal Microbiota Transplantation, to cure Clostridium difficile infections. |
 |
Dietary intervention alters the microbiota and its byproducts improving patient’s outcomesInflammatory bowel diseases (IBD) are chronic disorders of the gastrointestinal tract that may be caused by inappropriate inflammatory responses to normal intestinal microbes, collectively called microbiome- in a genetically susceptible host. Several genes involved in the body’s immune response seem to predispose for IBD but genes alone can't explain the sharp rise in IBD incidence. Now we are looking at environmental conditions that can promote the development of the disease. Increasing evidence support that IBD patients exhibit an altered microbiome (harmful bacteria outnumbering the beneficial ones), which can be the lost piece of the puzzle. Given the increasing evidence of the role of diet in shaping the microbiome we aim to understand how diet could restore the microbiome in such a way as to reduce disease activity and improve outcomes for patients suffering with IBD. Suggested recipies for IBD patients |
Mathematical modeling of microbiome dynamics to minimize the incidence of enteric diseasesEnteric infections represent a critical issue in today’s healthcare due to the increase in incidence and in the cost of eradicating them. Often these are due to a reduced colonization resistance against pathogens due to antibiotic-mediated killing of the protective native intestinal bacteria. In this project a combination of recently developed and new mathematical modeling frameworks, metabolic pathway reconstruction, and in vitro anaerobic experimentation is used to predict the risk of enteric diseases and to prototype rationally-designed fecal transplantation strategies for risk minimization. |
|
 |
The gut microbiome and different outcomes in multiple sclerosis progressionMultiple Sclerosis (MS) is a disabling central nervous disease. Laboratory studies have suggested that there may be a link between the bacteria in the intestine and the development of the disease. We are attempting to identify microbial markers that can be correlated with multiple sclerosis disease progression in an effort to understand how microbes may influence each stage. |
 |
Microbiota dynamics and function in conferred protection by vaccine against enteric bacteria.Objective: We aim to understand the role of the gut commensal bacteria in the protection obtained by inoculation with a suitable vaccine for diarrheal illness. Increasingly evidence has unveiled the crucial role of the microbiome on the development and training of our immune system. Several diseases such as inflammatory bowel disease, allergy/asthma, obesity and diabetes are associated with drastic changes on the bacterial community inhabiting our colon, intestines and skin to name a few. More recently, studies have found that the microbiome can influence the development and fate of immune cells, which ultimately will affect the response of our immune system towards infectious agents but also might play a role on the immunity promoted by vaccination. In this project we aimed to understand how the intestinal microbes can influence the protection conferred by an attenuated strain that have shown to prevent disease against Salmonella infection. |
 |
Prospecting in the rainforest to develop biofuel technologyPlant biomass is the most abundantly available source of renewable energy on Earth. Most of this energy is stored as lignocellulose, a polymer that is the structural building block for plants. Some bacteria are able to convert (or decompose) lignocellulose to biofuels. Bacterial communities in tropical forest soils exhibit some of the highest decomposition rates in the world. We study these soil microbiomes to understand and identify efficient and cost-effective processes for renewable energy production from plants. |
 |
Antibiotic-associated diarrhea and Clostridium difficile infectionsAntibiotics are important tools for treating infections. Antibiotics kill ‘bad’ bacteria but also kill the ‘good’ bacteria in your microbiome. When the good bacteria are disrupted, the imbalance affects the normal functioning of your gut and can lead to diarrhea and the overgrowth of ‘bad’ bacteria such as Clostridium difficile. By understanding how antibiotics harm the ‘good’ microbiome we can learn how to prevent diarrhea and Clostridium difficile infections. |
The Microbiome and ObesityOne of the more important functions of the microbiota is to aid in digestion. For example, ruminants such as cows have multiple stomachs to serve as bioreactors where specialized populations of bacteria break down the otherwise-indigestible starches found in grass. Within the human intestine, the gut microbiota is responsible for vitamin biosynthesis and harvesting inaccessible nutrients to produce bioavailable nutrition for the human host. This is a truly mutualistic relationship, in that the bacteria and the host benefit by providing for each other's nutrition. |
|
Role of the microbiome in regulating pro- and anti-inflammatory lipids in the intestineThe bacteria living in the human gut have a major influence on health and disease by giving off a variety of different signals. Dangerous bacteria such as Salmonella give off signals that can lead to inflammation, whereas beneficial members of a healthy microbiome work to maintain balance and prevent inflammation. We are trying to understand how human host cells interpret these signals and use them to “decide” how to respond. |
|
Disruption of enterohaemorragic E. coli biofilm formation through long-term experimental evolutionAntibiotic treatment to cure enterohaemorragic Escherica coli (EHEC) infections is often discouraged due to selection for antibiotic-resistant bacteria. The long-term goal for this project is to determine less evolutionary “cheatable” strategies to be used as alternatives to antibiotics. We combine experimental evolution assays and bacterial genomics to identify genetic modifications that result in altered traits, such as cell adhesion, infectivity, and biofilm formation. |
|
Bacterial metabolites controlling immune cell functionBile acids are cholesterol-derived, natural surfactants, produced in the liver. They are critical to lipid digestion, antibacterial defense, and cholesterol synthesis, as well as other aspects of human biology. Importantly, bile acid dysregulation has been linked to intestinal bowel disease. |
|
The microbiome and immune functionDiseases such as inflammatory bowel disease, allergy, asthma, obesity, multiple sclerosis, and diabetes are associated with drastic changes in patient microbiomes. In some cases, these changes are thought to contribute to or trigger the disease. For example, people with inflammatory bowel disease are thought to have pre-existing genetic risk factors that are triggered by environmental factors, leading to full-blown disease. An imbalance in the makeup of the intestinal bacteria may be one of these environmental triggers. Similarly, recent studies in mice have shown that the development of diabetes is affected by the presence of bacteria in the intestine. This is an especially interesting finding, because it suggests that intestinal bacterial colonization can have important effects on inflammation at sites far away from the intestine. |
|
Infectious DiseasesOne of the most important beneficial roles of the microbiome is its ability to protect against infection with dangerous microbes from the environment. The bacteria in the gut protect the integrity of our intestines by both passive and active means. It seems that friendly bacteria actually "talk" to the cells in the intestine, communicating when there are breaches to be repaired. These bacteria also talk to gut immune cells, preventing inflammation and promoting tolerance of the surrounding environment. At the same time, the simple presence of friendly bacteria helps prevent more dangerous microbes from causing disease. Competition with friendly bacteria for space and nutrients in the intestine is a major hurdle for harmful bacteria to overcome, and they often don't succeed. The importance of this passive protection by friendly bacteria is illustrated by the alarming example of antibiotic-induced diarrhea, which poses a severe threat to hospital patients. C. difficile is a bacterial species that normally lives quite happily in the intestine without causing problems, but is largely resistant to antibiotic treatment. Long-term antibiotic treatment kills other friendly bacteria, upsetting the normal balance and allowing rampant growth of C. difficile. Given free reign in the intestine, the bacteria cause severe diarrhea with potentially serious complications including death. The microbiota are therefore crucial for normal and healthy intestinal function and protection against pathogens. |
