 |
|
|
Jerry Gurwitz, MD |
|
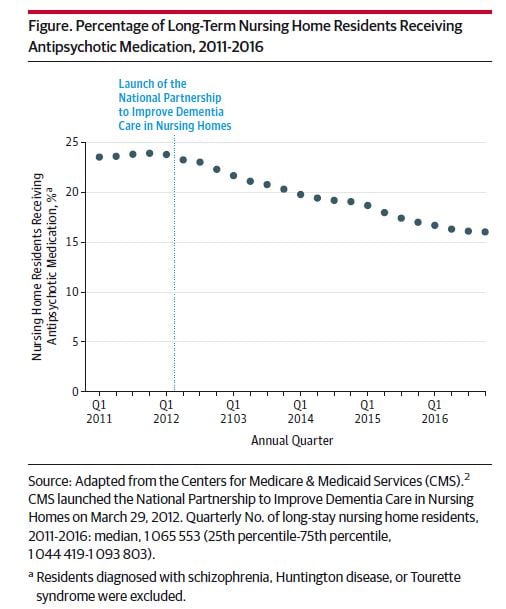 |
There has been a dramatic improvement in the past five years in reducing the excessive use of antipsychotic drugs in nursing home residents with dementia, according to a JAMA Viewpoint article published June 15.
Excessive use of antipsychotics in nursing homes has been a problem since the 1970s, according to Jerry Gurwitz, MD, the Dr. John Meyers Professor of Primary Care Medicine, and professor of medicine and family medicine & community health. Dr. Gurwitz, Alice Bonner, PhD, Massachusetts Secretary of Elder Affairs, and Donald M. Berwick, MD, president emeritus and senior fellow at the Institute for Healthcare Improvement and former administrator of the Centers for Medicare & Medicaid Services, co-authored the Viewpoint article.
It details the results of a national partnership to improve dementia care in nursing homes that was developed after a widely publicized 2011 Office of the Inspector General report found that more than one in five nursing home residents were being treated with antipsychotic drugs for behavioral symptoms of dementia, which is not an approved indication for these medications. When given to patients not suffering from mental health problems, these drugs can increase the risk of confusion, dizziness, over-sedation, falls and even death.
“The Centers for Medicare and Medicaid Services (CMS) initiative enacted a partnership focused on protecting nursing home residents from being prescribed antipsychotic medications unless there was a valid clinical indication, and there was an evaluation of each resident’s need for the drug,” Gurwitz said. “It is impressive that these efforts have led to a 33 percent reduction in antipsychotic drug use in nursing homes nationally in the past five years. In Massachusetts, there was also a 33 percent reduction. This is a remarkable success story that shows that the quality of care and medication safety in nursing homes can be improved on a national level.”
While this CMS initiative has been successful, according to Gurwitz, there is a need to further analyze why it worked, so that it can serve as a blueprint for future quality improvement efforts in nursing homes.
“We need to better understand what parts of the initiative were most important, what other steps can be taken to make care even better and how the strategies can be applied to improve care for older adults with dementia in other health care settings,” Gurwitz said.
The full JAMA Viewpoint can be read here: http://jamanetwork.com/journals/jama/fullarticle/10.1001/jama.2017.7032
Relates stories on UMassMedNow:
New study shows that antipsychotic medications can be reduced in dementia patients
In search of . . . safer medication use, Jerry H. Gurwitz