 |
|
| David Paydarfar, MD | |
 |
|
|
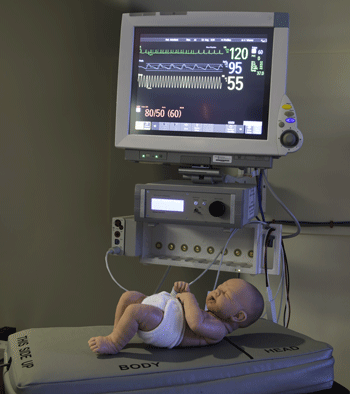
A new vibration-based prevention technology tested in a NICU reduces apneic events and improves critical clinical parameters in prematurely born infants. |
Scientists and clinicians at UMass Medical School, Wyss Institute for Biologically Inspired Engineering and the Beth Israel Deaconess Medical Center (BIDMC) have shown in a clinical trial that a new vibration-based prevention technology tested in a neonatal intensive care unit (NICU) reduces apneic events and improves critical clinical parameters in prematurely born infants. The apnea prevention system, initially conceived at UMass Medical School, was developed at the Wyss Institute and tested in a trial conducted at the BIDMC. The findings are reported in the November 23 issue of Pediatrics [doi: 10.1542/peds.2008-1536].
In the United States, one in nine infants is born prematurely and many are at higher risk for apnea of prematurity (AOP), typically defined as a prolonged pause in breathing of at least 20 seconds. In fact, such apneic episodes occur in more than 50 percent of infants born prior to 37 weeks and in almost every baby of very low birth weight. The episodes can be life threatening. Even if treated in NICUs, they can result in insufficient oxygen delivery to critical organs such as the brain, which is suspected to cause developmental delays and long-term cognitive deficits.
“Apneic breathing and its associated risks is a major challenge in NICUs today, and can also lead to prolonged and expensive hospital stays. This prompted us to develop a non-invasive, non-pharmacological solution that can address the immature respiratory control in these premature infants,” said David Paydarfar, MD, vice chair and professor of neurology at UMass Medical School and a Wyss Institute associate faculty member, who was the scientific lead on the apnea prevention program.
While others were focused on the moment when the baby stops breathing, Dr. Paydarfar began investigating how to prevent apnea from occurring in the first place. More than a decade ago, he assembled a multi-disciplinary team of basic and clinical scientists at UMMS to figure out not only how sensory processing normally functions in respiratory control, but also how the system experiences problems in an immature infant.
Key to the infant apnea prevention technology is the principle of “stochastic resonance”—early work by the Wyss Institute’s Core Faculty member James Collins, PhD, has revealed the counterintuitive phenomenon in which the application of a small amount of “noise” to a complex biological system, such as the human body, increases the sensitivity of that system. Dr. Collins is also the Termeer Professor of Medical Engineering & Science at Massachusetts Institute of Technology (MIT) and professor of biological engineering at MIT.
Paydarfar applied this principle to the problem of AOP. In an early pilot study done at UMMS, he showed that adding “noise” in the form of a subtle vibration in the mattresses of premature infants helps to stabilize breathing and improve blood oxygenation without waking the infant. This suggested that a stochastic resonance approach could compensate for the infants’ still immature respiratory control system and could prevent dangerous apneic events from occurring.
“Our team subsequently developed a new mattress device designed to deliver the same level of therapeutic vibration that was found to be effective in Dr. Paydarfar’s previous studies while limiting the vibrations that would otherwise be delivered to the head of the infant,” said John Osborne, a senior staff engineer at the Wyss Institute who co-conceptualized the new study and co-authored the publication.
The team has now validated this new mattress device in the BIDMC trial, in a cohort of 36 preterm infants who each had at least one previous event of apnea. The results of the trial provide comprehensive clinical evidence for the method’s ability to benefit breathing stability.
“By applying alternating intervals of 30-minute therapeutic mattress vibrations with 30-minutes of no vibration, we compared the effects of stimulation to the control period. During the therapy period, we saw a reduction in the incidence of apnea by 50 percent, and, perhaps equally important, we ameliorated every aspect of clinically significant oxygen desaturation events as well as demonstrated reductions in the severity of bradycardia. The technology therefore might be used as a stand-alone or as a supplement to the caffeine therapy that premature infants are commonly treated with,” said Vincent Smith, MD, MPH, an assistant professor of pediatrics at Harvard Medical School and BIDMC, who is also lead author on the published study.
“By de-risking the infant apnea prevention technology, the Wyss Institute and its clinical partners have now advanced it to the stage at which it can be more widely tested and eventually deployed in hospital NICUs. The findings exemplify once more how our translation engine can provide finely tailored solutions that may impact areas of clinical need,” said Wyss Institute Founding Director Don Ingber, MD, PhD, who also is the Judah Folkman Professor of Vascular Biology at Harvard Medical School and Boston Children’s Hospital, and professor of bioengineering at the Harvard School of Engineering and Applied Science.