Thirty first-year School of Medicine students crowded into the UMMS Simulation Center last week to get a closer look at what being an emergency medicine physician is all about. Through a simulation workshop organized by the medical student-driven Emergency Medicine Interest Group (EMIG), participants learned three procedures common in the day-to-day activity of an emergency room: intubation, IV insertion and emergency ultrasound.
“The goal of this workshop is not to make anyone a master of the skills,” said Mitchell Li, SOM ’13, and one of four officers of the EMIG. Instead, he said, the event gives students a safe way to get “a taste of the most common clinical skills and get them interested in emergency medicine by giving them some exposure to clinical skills that, in first and second year, you don’t get a lot of since your head is in the books all the time.”
In one room, students gathered around a gurney to watch third-year resident Susan Ly, MD, perform an ultrasound on Li, who had volunteered to be the ultrasound model. “See, here is the pericardium,” Dr. Ly said, pointing out the white border around Li’s beating heart. “If this were a trauma, you might see a dark area here, indicating pooling blood.” Ly walked students through the typical brief ultrasound exam used in the emergency department when there is a suspicion of internal injury or internal bleeding. Students then took turns operating the probe and identifying Li’s heart and kidneys.
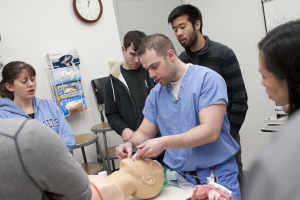
Second-year emergency medicine resident Jason Plansky, MD, uses a mannequin to demonstrate the proper placement of a breathing tube during a workshop held in the Simulation Center for first-year medical students.
In the intubation room, Constance G. Nichols, MD, clinical associate professor of emergency medicine, accompanied by second-year emergency medicine resident Jason Plansky, MD, supervised students as they practiced intubation—inserting a breathing tube—on a simulation mannequin. The procedure, which can be tricky and often needs to be done quickly to establish or preserve a patient’s airway, takes a steady and firm hand, but not too firm or “you could injure the patient or break his teeth.” Once the tube was placed, students could successfully inflate the mannequin’s lungs. One student commented that it was helpful to think of what they’d recently learned in anatomy class when practicing intubation.
At the last station—IV insertion—instructors guided students in properly handling needles and preparing the insertion site. Students first practiced on lifelike rubber arms that were tethered to IV bags full of simulated blood before pairing up and practicing on each other under the close supervision of their instructors, for whom IV insertion is an everyday task: emergency medicine resident Daisy Fischer, MD; David Derosier, RN; Andrzej Slezik, RN; and emergency medical technicians Matt Mullen and Chris Blood. Nearly every student rolled up his or her sleeve to offer a real-life practice site, although this part was optional.
Debra W. Heitmann, MD, clinical associate professor of emergency medicine, and faculty advisor for the EMIG, praised the interest groups—there are several across campus, including in family medicine, geriatrics and pediatrics—as a means of providing students with a better idea of what their career in a particular field might include. “The mission [of the EMIG] is to promote the idea of what emergency medicine is all about and to organize events around the specialty that are educational and informative,” Dr. Heitmann said.
Heitmann noted that the EMIG officers—second-year students Mitchell Li, Michelle Drever, Matthew Propert and Pardeep Thandi—have been resourceful and effective in planning the workshops and other events on campus, and in asking faculty and clinical staff to help. “They have wonderful ideas and come at this with a different perspective than an attending physician or an EMT might, so it’s a benefit not just to the students but to the faculty and staff who volunteer to help with the EMIG,” she said.
Related Links:
UMMS student groups and organizations
$12 million suicide-prevention study targets patients in the emergency room