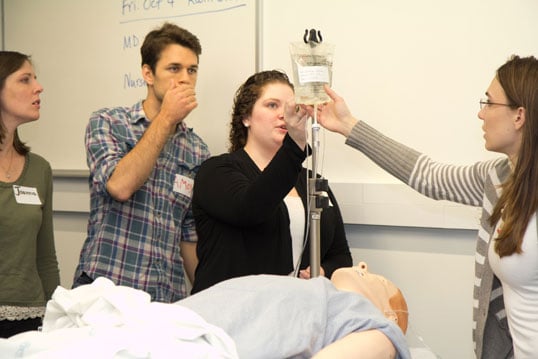
When the medical team entered the patient’s room, so many things were wrong. An uncapped syringe lying on the bed, dried blood on the floor, conflicting medication instructions and an allergy wrist band with no allergy identified were among the many obvious mistakes.
In real life this patient would be in serious danger. Luckily, the “patient” in this scenario was a simulation mannequin and the medical team comprised students engaged in a patient-safety learning exercise.
Dubbed “Room of Horrors,” the scene of the medical crime was a suite in the interprofessional Center for Experiential Learning and Simulation (iCELs) in the Albert Sherman Center, carefully staged by a team of medical educators intent on teaching medical and nursing students the necessity of interprofessional teamwork to ensuring patient safety.
“This is one in a series of interprofessional experiences that are part of the medical school curriculum,” said Melissa Fischer, MD, MEd, associate dean of undergraduate medical education. “The Room of Horrors experience was offered during patient safety month, to help improve students’ understanding of the roles on a team.”
Room of Horrors was coordinated by the Office of Undergraduate Medical Education to fulfill a second year medical education requirement for interprofessional learning and was developed with a grant from the Institute on Medicine as a Profession and Macy Foundations. Nursing students are not required to participate but most do since interprofessional learning experiences are a priority shared by both schools. Five rooms were set up identically to include 25 errors that posed a risk to the patient. The teams, which each included nursing and medical students, had seven minutes to record as many errors as possible.
Students are told all the time that the two essential elements for ensuring patient safety are team work and communication, but this hands-on activity created a realistic opportunity to put that lesson to the test.
“It was nice to be in a team with the medical students as well as be in a learning opportunity that was not in front of a PowerPoint presentation,” said graduate nursing student Lisa Buckley, whose team won a prize for finding the most errors. “I believe we were able to find multiple errors because we had someone step forward to lead the group who gave us a strategy before we entered the room. While we were in the room, people spoke to each other and felt comfortable giving ideas on what to do next.”
“We tried to create errors that would be noticeable to particular members of the team,” said Susan Collette, administrative assistant to Dr. Fischer, who coordinated all of the elements used in the scenario. The variety of errors staged helped reveal to the individual team members their own strengths and weaknesses, and reinforced the importance of interprofessional teamwork and communication.
“Many of our nursing student colleagues have more clinical experience on the wards and deal with patient safety on a more regular basis,” said third-year medical student Dylan Perry. “I was amazed by how quickly they picked up on errors that the medical students may have overlooked or taken longer to recognize. I was also surprised by how I could easily fall into the false sense of security in documentation validity. Being vigilant in double checking allergies, medications, dosing and other orders can absolutely prevent medication errors.”
Heather Galonzka, who is a graduate nursing student and registered nurse, sees first-hand that the patient safety lessons of the Room of Horrors come into play every day.
“I am a firm believer that teamwork on an interprofessional level will always yield better results for our patients. It is almost impossible for a single person to remember everything, but much more is remembered when more minds are involved. It is important to keep this in mind as we become clinicians.”