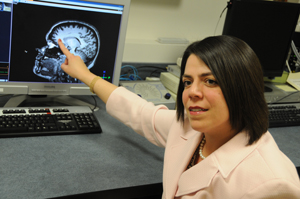
Psychiatrist and neuroscientist Kristina Deligiannidis, MD, is using brain scans like the one pictured here to learn why women develop post-partum depression.
Post-partum depression affects one in eight new mothers—many of whom don’t realize what is wrong until, weeks after giving birth, they are severely depressed, not bonding with their baby, even suicidal. But what if women at high risk for depression could be identified during pregnancy, so that their symptoms could be treated early or even avoided altogether?
“We want to be able to identify what the risk factors are, watch for the first symptoms before they’re in crisis mode, and be able to intervene before it’s harder to pull them out of it,” said UMass Medical School psychiatrist and neuroscientist Kristina Deligiannidis, MD.
With a new, five-year, $900,000 grant from the National Institutes of Health, Dr. Deligiannidis will use hormone and brain imaging investigations to learn why women develop post-partum depression.
“This is one of very few currently funded NIH grants that are dedicated to understanding the biological underpinnings of post-partum depression,” noted Deligiannidis, assistant professor of psychiatry and obstetrics & gynecology. “It will allow us to measure mood symptoms and hormones throughout pregnancy, and use specialized, multimodal brain imaging techniques available at UMass to understand how brain areas important for mood and behavior are connected and how hormones affect brain circuitry in those women who develop depression.”
The work will build on pilot studies made possible by seed funding from and collaboration between researchers in the Departments of Psychiatry and Quantitative Health Sciences and the Proteomic & Mass Spectrometry Facility at UMMS.
“We were struck by the extent to which our findings went beyond our initial hypotheses,” Deligiannidis said. “We demonstrated for the first time that mothers who developed the condition had much weaker communication, or connectivity, between several brain areas compared to healthy postpartum mothers. We also identified a hormone related to progesterone that may be abnormal in pregnancy in those women who later on developed post-partum depression.”
The ultimate goal for the neuroendocrine studies is to develop simple and inexpensive methods to detect, in pregnancy, those women at risk of developing postpartum depression.
“What we’re aiming to do in the long-run is to identify a biological marker of risk with an inexpensive blood test,” Deligiannidis said. “With early risk detection, we can be more proactive in supporting the pregnant woman at an individual and family level so that we can reduce her risk of developing depression in the post-partum period.”